When Your Child Has Juvenile Dermatomyositis
Juvenile dermatomyositis (JDM) is a rare disease that causes muscle inflammation and a skin rash. It's different from other muscle diseases because it also causes skin problems. Symptoms often first appear in children between ages 5 and 10. Children with JDM have weak muscles around the neck, shoulders, and hips. They also have a skin rash around areas such as the eyelids, knuckles, and finger joints.
How to say it
der-muh-toh-mi-oh-SI-tuhs
What causes juvenile dermatomyositis?
Healthcare providers don’t know the exact cause of this condition. But it may be linked to problems with the immune system that cause inflammation in the muscles and blood vessels.
Symptoms of juvenile dermatomyositis
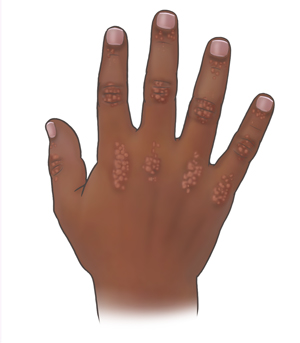
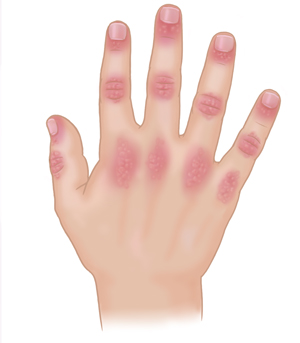
JDM symptoms often appear slowly over time. In some cases, they may happen more quickly or severely. Each child’s symptoms may vary. The most common symptoms can include:
-
Fever
-
Violet or dusky red rash around the eyelids, knuckles, or finger joints
-
Rash on the elbows, knees, and ankles
-
Progressive muscle weakness
-
Lack of energy (fatigue)
-
Ill feeling (malaise)
-
Muscle pain and soreness
-
Irritable mood
-
Trouble swallowing
-
Weight loss, from trouble swallowing
-
Joint pain and inflammation
-
Hardened deposits under the skin (calcinosis)
-
Mouth ulcers
-
Muscles wasting away (muscle atrophy)
-
Muscles that become paralyzed in a contracted position
-
Voice changes
-
Stomach ulcers
Diagnosing juvenile dermatomyositis
Your child's healthcare provider will ask about your child's health history and do a physical exam. Your child may also have tests, such as:
-
Blood tests. These tests are used to check for antibodies, muscle enzymes, and signs of inflammation.
-
Electromyelogram. This is an electrical test that may be done to find nerve or muscle damage.
-
MRI. This test uses large magnets and a computer to look for inflammation in the body.
-
Muscle and skin biopsy. Tiny tissue samples are removed and checked under a microscope.
Treatment for juvenile dermatomyositis
Treatment will depend on your child’s symptoms, age, and general health. It will also depend on how bad the condition is. There is no cure for JDM. But the symptoms can be managed. The disease may go into remission. This means the symptoms will go away. Treatments may include:
-
Medicines. These are used to treat inflammation and skin symptoms.
-
Physical, speech, and occupational therapy. This can help to improve muscle function and strength.
-
An exercise program. This also can improve muscle function and strength.
-
Sunscreen. This helps prevent more irritation or damage to the skin.
-
Nutrition. A healthy diet will help support the body’s health during the disease.
-
Vitamins and other supplements. These can also help support the body’s health.
Talk with your child’s healthcare provider about the risks, benefits, and possible side effects of all treatments.
Possible complications of juvenile dermatomyositis
Many children will recover from JDM without any lasting problems. Some children may have trouble moving because of shortening of the joints (contractures). Other children may have ongoing (chronic) symptoms. These may include pain, muscle weakness, and delayed growth. There may be damage to bones, joints, lungs, and other internal organs.
Living with juvenile dermatomyositis
JDM can make it hard for a child to take part in school and other activities. Work with your child’s school to help teachers and caregivers understand your child’s limits. A healthy lifestyle can help improve your child’s quality of life. This includes a good diet, exercise, and rest. A support group may help your child feel less alone or different.
When to call your child’s healthcare provider
Call the healthcare provider if your child has any of these: